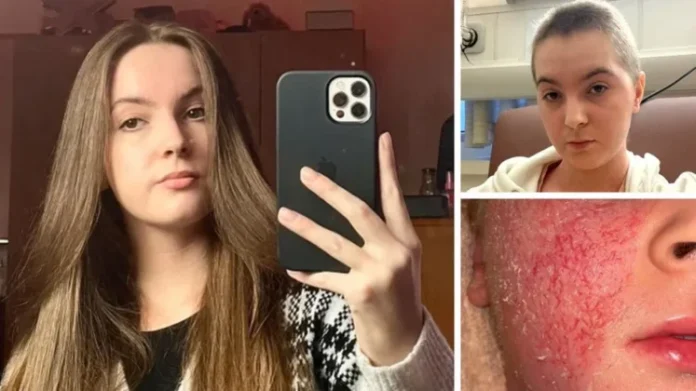
For years, steroid creams kept Bethany Gamble’s eczema under control. From the age of two, they were a reliable part of her life. Then, at 18, everything changed.
Small patches of eczema in the creases of her elbows and behind her knees began to spread. Her skin became hot, inflamed and red. It cracked, oozed and itched “bone deep”.
By the time she turned 20, the pain was so severe she could not get out of bed. Her mother had to take time off work to care for her. But for the 21-year-old from Birmingham, the hardest part was not being believed.
“I was constantly gaslit by doctors,” she said. “They kept telling me it was just my eczema and offering me more steroids. I’ve had eczema my whole life – this was different.”
Bethany is among a growing number of people documenting their experiences online under the hashtag TSW – topical steroid withdrawal. Videos on TikTok bearing the hashtag have been viewed more than a billion times.
Also known as red skin syndrome, TSW remains so under-researched that some GPs and dermatologists struggle to diagnose or treat it. While some experts believe it is a debilitating reaction to steroid creams – the first-line treatment for many of the eight million people in the UK with eczema – others argue it is simply a severe flare-up of eczema or other skin conditions, and question whether it exists at all.
Now, the first UK research of its kind is under way, prompted by the surge of online testimonies and the experiences of patients whose symptoms do not fit existing medical understanding.
Professor Sara Brown, a consultant dermatologist at the University of Edinburgh, secured funding from the National Eczema Society after witnessing “unexplainable” symptoms in her own patients and the desperation evident in social media posts.
“We’re seeing patterns in TSW that cannot be explained by what is known about eczema,” she said. “Symptoms like thickening and laxity of the skin, so-called ‘elephant skin’, extreme shedding and sharply defined areas of redness next to normal skin.”
Alongside co-researcher Dr Alice Burleigh from Scratch That, a TSW patient group, Professor Brown has recruited hundreds of participants across the UK to analyse symptoms, saliva samples and skin biopsies in an effort to understand why some people develop the condition and others do not.
Henry Jones, 22, from High Wycombe, is among those taking part. A self-described “TSW warrior”, he said his symptoms became so severe he had to drop out of his university degree.
“My GP at university kept telling me it was just eczema – and kept prescribing me more steroid cream,” he said. “Something didn’t feel right.”
The more cream he used, the worse he felt. His skin became red, tight and flaky before oozing and starting the cycle again. As the patches spread across his body, he could no longer go outside, socialise or study. At points, he said, he wanted to take his own life.
For people with darker skin, the condition can be even harder to identify. While TSW appears as an intense red on white skin, on black or brown skin it may show as deep purple, brown or a greyish tinge.
Karishma Leckraz, 32, from Kent, said she spent years in denial because her symptoms looked markedly different from the images posted by white people on social media.
“TSW took everything away from me,” she said. “I had to hide from the world for so long. My skin was so bad, the pain, the lack of sleep, just not recognising myself.”
She stopped using steroid creams five years ago and said her skin has largely healed, though she still struggles with social anxiety.
Andrew Procter of the National Eczema Society said patients were “stuck between a rock and a hard place”.
“We know that steroids work for the many millions who use them,” he said. “But we also have a condition that at the moment, can’t be explained, which is causing real fear – and that is completely understandable. That is why more research is desperately needed.”
For those experiencing TSW-like symptoms, accessing treatment can be a significant challenge. GPs may refer patients to dermatologists, but waiting times often exceed a year. For most, steroid creams remain the only option.
At the Royal London hospital, consultant dermatologist Dr Alia Ahmed runs a specialist NHS clinic offering alternatives including psychological support, immunosuppressants and phototherapy.
“The psychological impact, as well as the physical effects, is huge,” said Dr Ahmed, a member of the British Association of Dermatologists. “We have to work with the patient to understand the best course of treatment for them.”
The Medicines and Health Regulatory Authority officially recognised TSW as a severe reaction to steroid creams in 2021, but considers the condition relatively rare. It warns that long-term use can lead to side effects including skin thinning, adrenal suppression and, in very rare cases, Cushing’s syndrome.
The Royal College of GPs said steroid creams were a “safe and effective treatment for many skin conditions”, but acknowledged that in “rare cases” people may experience reactions linked to “long-term or inappropriate use”. It advised patients to speak to their GP if concerned and not to stop medication without medical advice.
For those whose lives have been upended by the condition, the path to recovery has often been long and uncertain.
Rebecca Ebbage, 32, said her skin became her “ruler” after she stopped taking topical and oral steroids in July 2022 following a severe flare. After waiting a year for a dermatology appointment and trying multiple immunosuppressants with little success, she turned to private Cold Atmospheric Plasma therapy, a relatively new treatment not officially recognised by the NHS. After nearly a year, she said she was beginning to recover.
Henry received an official diagnosis in August 2025 and is now under the care of a TSW specialist at the Royal London, taking immunosuppressants and feeling “normal again”.
Karishma has become an advocate for those with debilitating skin conditions, appearing in marketing campaigns on social media and billboards.
Bethany is now taking biologics – a newer type of medication that targets inflammation – and has recently secured her first job.
“Do not feel guilty, do not feel like it’s your fault – and fight to be believed,” she said.